Our Story
By tapping our deep experience in practical, patient-centered research, we're accelerating care transformation to improve health for all people and communities.
Realizing our vision for care transformation — and taking it to new heights
The ACT Center was established in 2021, but our story starts long before then and has roots in some of our nation’s earliest efforts to transform care through collaborative, patient-centered approaches to research.
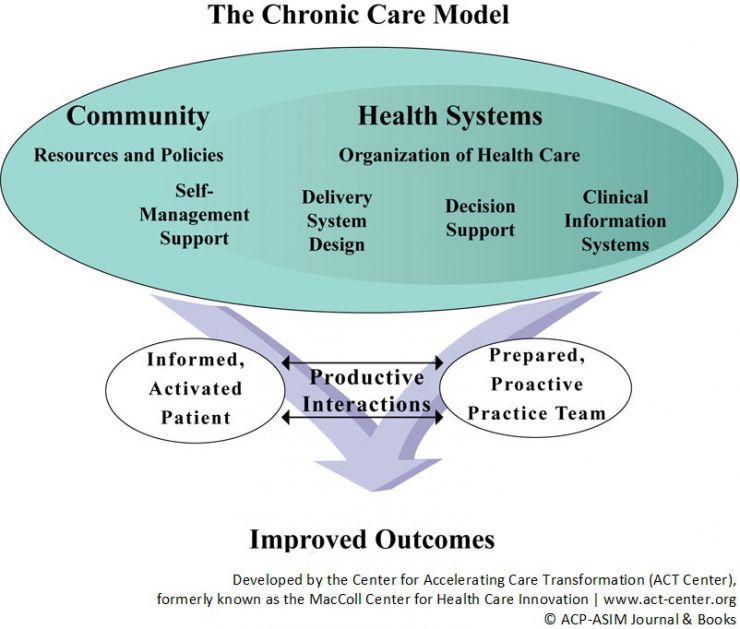
- Founded by Dr. Ed Wagner in 1992, the MacColl Center became known as a global pioneer in care transformation after developing and supporting the wide-scale adoption of the Chronic Care Model, with a special focus in safety net settings. The Chronic Care Model and other tools created by the MacColl Center are used worldwide and have been translated into dozens of languages.
- Our home institution, Kaiser Permanente Washington Health Research Institute (KPWHRI), has long been a pioneer in taking the learning health system (LHS) model from concept to action — dating back to its days as Group Health Research Institute (part of Group Health Cooperative). The LHS approach uses research to improve health and health care for diverse populations. This means working with patients, care teams, and health care leaders to help health care organizations make patient-centered decisions that are informed by science, driven by their own data, and designed to be sustainable.
- When Group Health became Kaiser Permanente Washington in 2017, KPWHRI was charged with putting our scientific capabilities to work to help health system leaders use timely, rigorous, and patient-centered approaches to solve their most pressing problems. As a result, Kaiser Permanente Washington formalized the Learning Health System Program to bring its researchers, patients, and care teams together to find practical, equitable, and evidence-based ways to improve care.
- Our deep partnership with Kaiser Permanente Washington enabled us to become leaders in training LHS scientists, starting with the CATALyST program in 2018 and leading to the ongoing Washington LHS E-STAR training program.
- In 2021, the LHS Program and the MacColl Center combined into a new center focused on transforming care at Kaiser Permanente and beyond. The Center for Accelerating Care Transformation — or ACT Center — was launched that year, expanding the team’s capabilities, partnerships, and impact while preserving and enhancing their shared vision of better health for all people and communities.
This rich history makes the ACT Center a leader in care transformation and translation of evidence to practice. As the ACT Center continues to evolve to meet new challenges in health care and health research, the tenets that guided the LHS Program and the MacColl Center hold true:
- Our work is rooted in embedded research and using a rigorous, evidence-based, data-driven approach to transforming care. This rigor includes an emphasis on state-of-the-art implementation methods to ensure lasting change.
- Our teams are impatient to act at scale — meaning we’re not content with incremental change. If we have a best practice in hand, we are tenacious about finding ways to scale it up quickly, so it can transform care and improve health.
- We are motivated by the goal of eliminating health disparities — seeking to elevate the patient voice, in the service of higher quality and more equitable care.
- We are committed to co-creation, and we conduct all our work in close partnership with the people who are closest to the challenges we’re aiming to overcome. This includes patients and families with valuable lived experience managing their health and the care teams who work hard every day to provide the best care possible.